eHealth Technologies Blog: Michelle Donowsky, RT(T), Executive Director of Clinical Optimization, eHealth Technologies

The PSAW theme for this year is “We all play a role in healthcare safety.” That could not be more true when I think about the important role eHealth Technologies plays in assisting hospitals across the country gather medical records and prepare for a referred patients’ first appointment. Patient safety and security are at the forefront of everything we do. One of the most pertinent areas of patient safety we deal with is accuracy in patient identification.
In the spirit of PSAW, this is a great time to reflect on processes and safeguards in place to ensure that patient safety is never compromised during the medical record, image, and pathology slide collection and organization process at eHealth Technologies.
Requesting records for the right patient: Demographic Integration
Starting right at the beginning – when a request is made – Demographic Integration provides staff with the ability to eliminate patient identification errors because it leverages data directly from the hosptital EMR using the ADT (Admission/Discharge/Transfer) feed. This means there is less of a chance that the wrong patient will be identified for a records request as all patient demographics are identical to what is included in the EMR.
Receiving records for the right patient: QA Times Three
As requested records are sent from providers to eHealth Technologies, our operations team executes a three prong QA process to ensure that the records are in fact, associated with the correct patient.
- The first step utilizes our robust OCR (Optical Character Recognition) technology along with specific patient demographic matching algorithms to detect two patient identifiers on each page of the medical record. If there is missing information detected on a particular page or pages, a red flag is put in place for the second review.
- Part two of the QA process involves eyes on each page. If there is missing or conflicting information, the provider is contacted for verification.
- Once all records from each provider have been complied and organized, a third check is executed before the patients’ records are passed to the requester.
Delivering records for the right patient: Clinical Document and Image Integrations
By implementing different Integration solutions, our customers receive the benefit of automating the medical record and image delivery process. Without an automated process, staff are dealing with print outs, scanned files, or CDs that need to be meticulously organized to ensure they are either added to the correct patients’ paper record or uploaded to the correct patient record in the EMR/PACS. Each patient could have dozens of images or hundreds of pages of records sent to complete their record. Given high patient volumes, staff could be dealing with a multitude of patients each day. The opportunity for error in this scenario can be eliminated by automating the process of having organized records and images delivered directly into the EMR and PACS. This also removes the manual burden staff face as requested patient information is delivered.
Identifying the right clinical information: Keywords in an Indexed Medical Record
The indexed document that our team delivers through Intelligent Clinical Record services has several unique features that assist clinicians in the record review process.
- The first is that records are organized by record type, in reverse chronological order. From the cover page of the document, clinicians can easily click on the record category to navigate directly to that section.
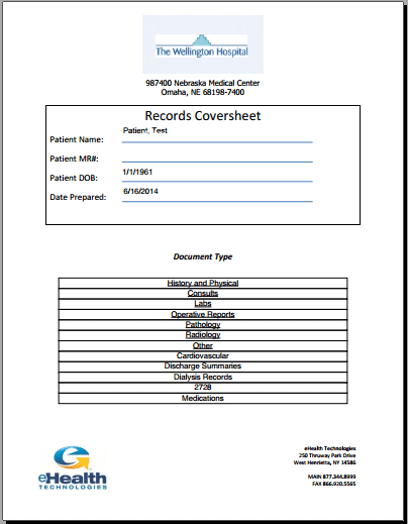

- Second, pertinent key terms (determined by the clinicians we work with from each specialty) are highlighted throughout the document. This makes a term, such as “hemophilia” for a patient referred for surgery, easy for clinicians to identify as they scroll through the document.

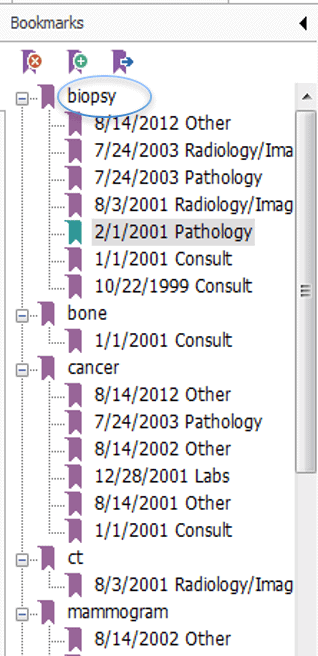
- And finally – the document is set-up to ensure key terms are bookmarked by service date and record type, giving clinicians another easy way to locate important information.

These features all contribute to ease of navigation and quick access to the relevant information needed to create the best possible care plan, with the least patient risk. Bringing critical medical indicators (allergies, current conditions, and previous treatments) to the forefront could change the course of treatment recommendations and prevent medical errors.
We recognize that as health care providers and facilitators, we should take the time to reflect on the importance of PSAW this month. Our processes and systems, along with diligence and attention to detail from our 200+ member team, allows us to proudly partner with health systems and hospitals to provide the best possible care for patients. Together – “we all play a role in healthcare safety.”
P.S. – Need a mental break this week? Check out this patient safety word search puzzle from the American Society for Health Care Risk Management. Have fun!